Dry mouth, also known as xerostomia, is a common condition that occurs when the salivary glands do not produce enough saliva to keep the mouth moist. While xerostomia is often temporary and can be caused by factors such as dehydration, medication side effects, or breathing through the mouth, there is emerging evidence of its association with long-term symptoms of Covid-19. In this blog, we will explore the connection between dry mouth and long term Covid symptoms, the prevalence of dry mouth in long Covid patients, the impact of dry mouth on daily life, coping strategies, and available treatment options.

Understanding Dry Mouth as a Long-Term Covid Symptom
Dry mouth, also known as xerostomia, is a common condition that occurs when the salivary glands in the mouth do not produce enough saliva to keep the mouth moist. It can be caused by several factors such as medication side effects, dehydration, or underlying medical conditions like Sjogren’s syndrome. However, recent studies have shown that xerostomia may also persist as a symptom of long term Covid. While the exact reason behind this connection is still unclear, it is believed to be related to the virus affecting the salivary glands and disrupting their normal function. Patients with persistent dry mouth due to Covid are advised to stay hydrated and use artificial saliva substitutes to alleviate discomfort.
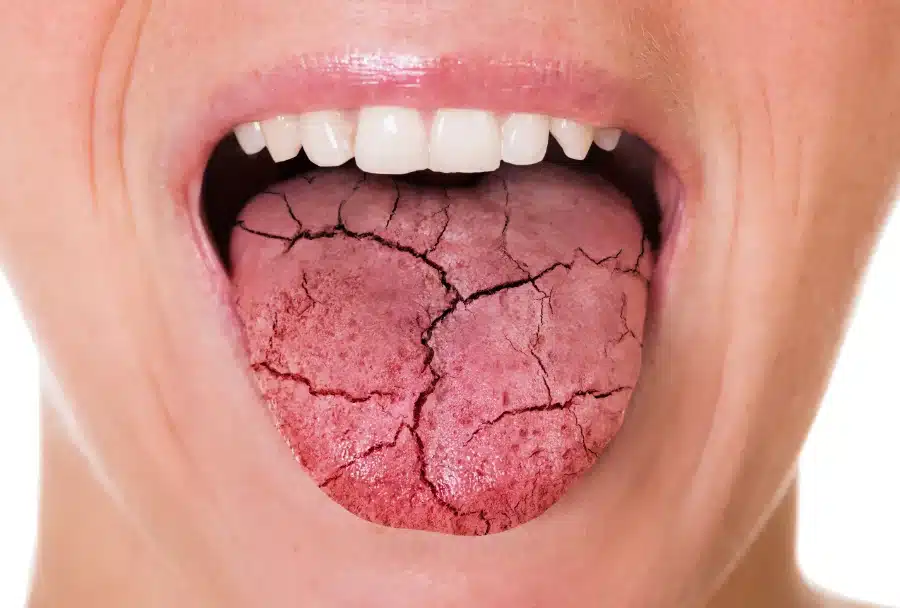
What is Dry Mouth?
xerostomia is a condition that arises when the salivary glands do not produce enough saliva, resulting in a dry and sticky feeling in the throat, mouth and tongue. It can cause discomforts such as difficulty swallowing and chewing, hoarseness or sore throat. When dry mouth persists as a symptom of Covid-19 over an extended period of time, it can severely affect an individual’s quality of life and daily routine. To alleviate the symptoms of dry mouth caused by Covid-19, individuals can drink plenty of water to stay hydrated and suck on sugar-free candies or chew gum to stimulate saliva production. In severe cases, medication may be prescribed to increase saliva flow or address underlying health conditions contributing to dry mouth.

Connection between Dry Mouth and Covid-19
Research suggests that there may be a link between long term symptoms of Covid-19 and dry mouth. The virus may have long-term effects on salivary gland function, resulting in persistent dry mouth. Further investigation is needed to fully understand the connection between Covid-19 and dry mouth. It is important for healthcare providers to be aware of potential long-term effects of Covid-19, including dry mouth, to provide comprehensive care to patients.

What are Other Long Term Covid-19 Side effects
Long COVID is a term used to describe symptoms that persist or develop after the initial COVID-19 infection, and it can include shortness of breath as well as other symptoms such as fatigue, cognitive problems, chronic pain, and heartbeats that can become noticeable (palpitations). It is important to seek medical attention if you experience any of these ongoing symptoms, whether they are related to COVID-19 or not. The most common symptoms of long COVID are extreme tiredness (fatigue), feeling short of breath, loss of smell, muscle aches, and problems with memory and concentration (“brain fog”). Additionally, risk factors for Long COVID can also occur after a COVID-19 infection. Mental health problems can arise from grief and loss, unresolved pain or fatigue, or from post-traumatic stress disorder (PTSD) after treatment in the intensive care unit (ICU).

Respiratory symptoms such as cough, shortness of breath, and difficulty breathing can be associated with COVID_19. Additionally, dry mouth may occur because of breathing through your mouth due to shortness of breath or the use of a breathing machine. This can leave you with an unpleasant feeling in your mouth and throat, which can be alleviated by drinking water or using a humidifier. It is important to note that while dry mouth is not a commonly reported symptom of COVID-19, it is possible to experience this symptom along with other respiratory symptoms. If you suspect that you may have COVID-19 or are experiencing any concerning symptoms, seek medical attention immediately.

Chronic fatigue syndrome (CFS) is one of the conditions that can develop after a COVID-19 infection and shares some similarities with COVID-19 syndrome. CFS involves extreme fatigue that worsens with physical or mental activity and does not improve with rest. Additionally, some people with COVID-19 may experience digestive symptoms such as diarrhea and stomach pain, which are also common in CFS. The symptoms are similar to those reported by people with myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS) and other poorly understood chronic illnesses that may occur after other infections. While most people’s symptoms gradually improve over time, some may experience symptoms for weeks, months, or even longer. Long COVID can also trigger other health conditions, such as diabetes or kidney disease.

Heart rate fluctuations can be an indicator that you have contracted the virus and after. During your visit you will have your blood pressure and other vitals checked during a medical examination. If you suspect that you may have COVID-19 or long term covid, it is important to speak to a healthcare professional as soon as possible and receive proper diagnosis and treatment. Your heart rate may also need to be monitored if you are experiencing symptoms of postural tachycardia syndrome (PoTS), which can be a complication of long COVID. The heart damage is caused by the inflammation the virus triggers, not the virus directly infecting the heart. About a third of patients who are hospitalized for COVID-19 have evidence in their blood tests of injury to their hearts, said Peter Libby, MD, a cardiologist at the Brigham. We understand from research at the Brigham that this damage isn’t the result of the coronavirus directly infecting the heart. In October, the Brigham launched a national clinical trial that aims to prevent the development of blood clots in patients with enduring symptoms of COVID-19. Dr. Connors is the study’s national principal investigator; Paul M. Ridker, MD, MPH is the trial’s chairman. Research is ongoing about how long COVID affects people who had breakthrough COVID, but it is likely that being vaccinated reduces the risk of hospitalization.
Mental health conditions such as anxiety, depression, and post-traumatic stress disorder (PTSD) have been linked to the virus. The pandemic has caused widespread stress and uncertainty, leading to an increase in mental health issues among the general population. It is important to seek medical help if you are experiencing mental health symptoms related to COVID-19 or otherwise, as there are many services available that can help manage your symptoms and support your recovery from cognitive impairment after acute coronavirus infection. For individuals with physical mobility problems, physical therapy can be beneficial in improving their mobility and overall function.

Headaches and dizziness; some individuals may experience headaches and dizziness as medium to long-term symptoms following COVID infection, as noted by Neurologist Arun Venkatesan. Despite ongoing research, the cause of these symptoms remains unclear. These symptoms are not limited to COVID-19; they can also be a result of other respiratory viruses. Additionally, some people who have recovered from COVID-19 may experience post-viral fatigue syndrome which can lead to persistent headaches and dizziness. It is important for individuals experiencing these symptoms to consult with a healthcare professional for proper diagnosis and treatment.

POTS and Insomnia after COVID-19
While dry mouth is a common symptom of COVID-19, some patients may experience more severe symptoms after they have been infected. Postural orthostatic tachycardia syndrome (POTS) and insomnia are two such examples. POTS is a condition in which the heart rate increases abnormally upon standing up, causing dizziness, lightheadedness, and other symptoms. Insomnia is another possible symptom, which can result in difficulty falling asleep or staying asleep throughout the night. These symptoms can be managed with proper medical care and attention from healthcare professionals.

Kidney Damage from COVID-19
Kidney damage is a serious concern for those who have contracted the virus. Studies have shown that kidney damage can occur in up to 30% of patients with severe cases of COVID-19. The virus can cause inflammation and damage to the kidney tissue, leading to decreased kidney function and potential long-term health complications. It is important to monitor kidney function and seek medical attention if any symptoms arise. Additionally, Brigham neurologists Tanuja Chitnis, MD, and Maria Houtchens, MD, have launched a trial to examine how COVID-19 influences the immune system in patients with multiple sclerosis (MS). The trial assesses the short and long-term outcomes of COVID-19 infection in MS patients and how certain immunotherapeutic treatments used to treat MS impact COVID-19 outcomes.
Bhattacharyya is launching a study that will use advanced imaging, such as magnetic resonance imaging (MRI), to examine the brains of patients who’ve recovered from COVID-19. The study will use the Brigham’s 7 Tesla (7T) MRI scanner—one of only a few in the country to be approved for clinical use—and functional MRI (fMRI) to examine functioning and connectivity in the brain. The NIH launched the Researching COVID to Enhance Recovery (RECOVER) Initiative in early 2021 to identify risk factors and causes of Long COVID to help understand how it can be prevented or treated in the future.

Long Term Covid Symptom of Xerostomia
Xerostomia has been reported as one of the long covid symptoms. Long covid symptoms refer to symptoms that persist long after a person has recovered from the initial covid infection. According to an international study published in EClinicalMedicine, there are about 200 long covid symptoms identified so far, and xerostomia is one of them. Other long covid symptoms include fatigue, shortness of breath, joint pain, and brain fog. It is important to seek medical advice if you experience any long covid symptoms.

The Prevalence of Dry Mouth in Long Covid Patients
Xerostomia is a common symptom experienced by long term Covid patients. This condition occurs when there is a decrease in saliva production, leading to discomfort, difficulty in swallowing and speaking, and an increased risk of oral health problems. The exact prevalence of xerostomia in long term Covid patients is still unknown, but studies suggest that it may be a common symptom alongside other long term effects such as fatigue, body aches, and brain fog. It is important for healthcare professionals to address this symptom and provide appropriate treatment options to improve the patient’s quality of life.

Research Findings on Xerostomia in Long COVID Cases
Current research is centered around comprehending the occurrence and significance of xerostomia in individuals with long term Covid. The objective of these studies is to offer valuable knowledge on how to effectively manage persistent symptoms, including dry mouth, that are linked to Covid-19. These scientific inquiries hold global significance as they illuminate the enduring consequences of Covid-19.

Demographics Most Affected by this Symptom
Certain demographics, such as older adults, may experience higher rates of dry mouth as a long-term symptom of Covid-19. Factors like gender, ethnicity, and underlying health conditions can influence the prevalence of dry mouth in long term Covid cases. Understanding the demographics most affected by long term symptoms, including xerostomia, is crucial for tailoring support and care for individuals.

The Impact of Xerostomia on Daily Life
Xerostomia, a common long term Covid symptom, can significantly impact daily life. It affects speech, sense of smell and taste, and the ability to comfortably consume food. Coping with persistent dry mouth may lead to social, emotional, and physical challenges for individuals managing long term Covid symptoms. Lifestyle adjustments and health care services are often necessary for those dealing with ongoing health problems. Understanding the broader impact of dry mouth is vital in providing comprehensive care to long term Covid patients. Embracing holistic support, the best way is to incorporate using Lubricity Dry Mouth Spray, can greatly benefit individuals experiencing this challenging symptom.

Challenges Faced by Individuals Experiencing Dry Mouth
Individuals with persistent xerostomia are at higher risk and may encounter difficulties in speaking, eating, and maintaining oral health. This condition can lead to discomfort, altered taste perception, and challenges with wearing dentures. Long term Covid patients coping with xerostomia face unique hurdles that require attention from healthcare providers. Supporting individuals in managing these challenges is crucial for their overall well-being. Moreover, the use of Lubricity Dry Mouth spray has been transformative for many people, offering symptomatic relief and improving their quality of life.

How Xerostomia Affects Oral Health
Xerostomia can contribute to an increased risk of dental decay, gum disease, and oral infections. The lack of saliva, which normally helps cleanse the mouth and neutralize acids, can lead to adverse effects on oral health. Long term Covid patients experiencing xerostomia symptoms should be aware of the potential implications it may have on their oral health and seek specialized care, if necessary.
Xerostomia can be caused by various factors other than COVID-19. Certain medications such as antihistamines, antidepressants, and diuretics can contribute to dry mouth. Additionally, medical conditions like diabetes, autoimmune disorders, and nerve damage can also cause xerostomia. To learn more about xerostomia and its causes, check out our blog section where we have covered home remedies and additional information on this topic.
Coping with Xerostomia: Practical Tips
Xerostomia can be a frustrating symptom that can be alleviated by staying hydrated and drinking water regularly. Other remedies include using sugar-free lozenges, chewing sugarless gum, or utilizing saliva substitutes for comfort. It’s also important to avoid substances like caffeine, tobacco, and alcohol that can worsen symptoms of xerostomia. Practicing good oral hygiene by brushing and flossing regularly is crucial to keep long term symptoms at bay. For individuals experiencing persistent xerostomia due to Covid-19, seeking guidance from healthcare providers is essential in managing the condition effectively. For more information on Conquering Dry Mouth check out this blog at Lubricity Innovations website.

Hydration and its Importance in Managing Xerostomia
If you’re struggling with Xerostomia, ensuring that you stay hydrated is crucial. Drinking water frequently can help alleviate the discomfort of xerostomia by promoting saliva production. Proper hydration not only helps relieve xerostomia symptoms but also supports overall oral health, reducing the risk of dental problems such as cavities and gum disease. It is recommended to drink at least eight glasses of water a day to maintain adequate hydration levels. Additionally, limiting caffeine and alcohol intake can help prevent dehydration and further aggravation of dry mouth symptoms.

Dietary Adjustments to Alleviate Xerostomia
- Making dietary adjustments can help alleviate Xerostomia symptoms.
- Consuming sugar-free candies or gum can stimulate saliva production, providing relief.
- Including moist foods like soups and stews in the diet can combat dry mouth as they provide additional moisture.
- Avoiding salty and spicy foods can alleviate discomfort associated with dry mouth.
- Chewing sugarless gum or sucking on ice chips can provide temporary relief.
- Lubricity Dry Mouth Oral Spray, in clinical trials show around 70% choose lubricity over competitor’s band
- Increasing intake of fruits and vegetables with high water content can ease dry mouth symptoms.

Medical Interventions for Dry Mouth in Long-Covid Patients
For individuals who have been dealing with persistent xerostomia symptoms as a result of long term Covid, medical intervention might be necessary. There are several treatment options available to alleviate the symptoms and improve quality of life. One such option is medication, like pilocarpine or cevimeline, which can stimulate saliva production. Over-the-counter Lubricity•, saliva substitutes and oral moisturizers are also available. In severe cases, doctors may recommend a procedure called salivary gland duct ligation or radiation therapy to reduce saliva production. It is important to consult with a healthcare professional before starting any treatment options to ensure they are safe and effective for your specific situation.

Is Dry Mouth a Symptom of COVID?
Dry mouth is a less common symptom of COVID-19, but it has been reported by some individuals. It is important to note that xerostomia can have various causes, so it is always recommended to consult a healthcare professional for a proper diagnosis if you are experiencing this symptom.
Can Dry Mouth Occur as the Only Symptom of COVID-19?
Yes, xerostomia can occur as the only symptom of COVID-19. While xerostomia is a common symptom of various conditions, it has been reported as a sole symptom of COVID-19 in some cases. It is important to get tested and seek medical advice if you experience xerostomia or any other concerning symptoms.

When to Seek Professional Help?
Long-term Covid patients should seek professional help if persistent dry mouth symptoms significantly affect their quality of life. Individuals experiencing severe symptoms, such as difficulty swallowing, should seek immediate care. If over-the-counter remedies do not alleviate dry mouth, long-term Covid patients should consult healthcare providers for effective treatment options. Seeking professional help is crucial in managing persistent dry mouth symptoms.

Treatment Options Available for Dry Mouth
Dry mouth can be a discomforting condition, but fortunately, there are different treatment options available. Saliva-stimulating medications, moisturizing mouth sprays, and gels, as well as saliva substitutes, are some of the popular choices for relieving dry mouth symptoms. For long-term Covid patients, these treatments can provide immense relief and support overall oral health. It is essential to collaborate with healthcare providers to find the most suitable treatment approach for individual needs. In addition to these remedies, certain lifestyle changes such as drinking plenty of water, avoiding alcohol and tobacco products, and maintaining good oral hygiene can also help manage dry mouth effectively.

Can Recovery from Dry Mouth be a Sign of Recovery from Long-Covid?
Dry mouth is a common symptom experienced by individuals with Covid-19, and improvement in these symptoms may indicate progress in long-term recovery. The relief of dry mouth symptoms is an encouraging sign as it suggests positive health developments. Regular monitoring of changes in dry mouth symptoms may provide insights into long-term recovery from Covid-19. This emphasizes the importance of identifying and addressing any lingering symptoms after the initial recovery period to ensure a full and complete recovery from the virus. Additionally, proper hydration and oral care can help alleviate dry mouth symptoms and support overall recovery efforts.

Conclusion
In conclusion, dry mouth is a prevalent and persistent symptom experienced by long-Covid patients. It can have a significant impact on their daily lives, affecting their oral health and overall well-being. Hydration and dietary adjustments play a crucial role in managing dry mouth symptoms. Seeking professional help is essential for proper diagnosis and treatment options tailored to individual needs. It’s important to note that recovery from dry mouth may indicate progress in recovering from long-Covid. If you are experiencing dry mouth as a long-term Covid symptom, don’t hesitate to reach out to healthcare professionals who can provide the necessary guidance and support. Remember, you are not alone in this journey towards better health.


